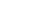A Vet’s Guide to Pododermatitis in Dogs 2025 🐾
In this article
A Vet’s Guide to Pododermatitis in Dogs 2025 🐾
By Dr. Duncan Houston BVSc
Hi, I’m Dr Duncan Houston BVSc, veterinarian and founder of Ask A Vet. Pododermatitis—paw inflammation—is painful, disruptive, and often challenging. In this vet‑approved guide, we’ll explore the multifactorial causes (infection, allergy, autoimmune, metabolic, trauma, tumors), recognize key signs, review diagnostic methods, map out treatment protocols, and share long‑term care strategies—including calming tools to support healing and comfort in 2025. 🩺🐶
1. What Is Pododermatitis?
Pododermatitis refers to inflammation affecting the paws—interdigital spaces, pads, and nailbeds. Common features include swelling, redness, ulceration, nodules, crusting, or discharge.
2. Common Causes 🩺
- Infections—bacterial, yeast, fungal, parasitic (e.g., demodex): often secondary to trauma or allergies.
- Allergies—environmental, food, contact: trigger paw chewing → inflammation/infection.
- Immune-mediated—e.g., pemphigus foliaceus, lupus: present with ulcers/crusts at nailbeds.
- Hormonal/metabolic—hypothyroidism, Cushing’s, hepatocutaneous syndrome: cause secondary skin infections.
- Trauma/irritants—hot pavement, foxtails, friction injuries.
- Tumors—e.g., nailbed melanoma or squamous cell carcinoma- often affect a single paw.
3. Who’s at Risk?
Any dog can develop pododermatitis, but predisposition includes breeds with skin folds or foot conformations—Bulldogs, Mastiffs, Boxers, Poodles, Labradors, German Shepherds, and those with obesity or arthritis.
4. Recognizing the Signs
- 🥾 Red, swollen, inflamed paws
- Constant licking, chewing, or biting
- Hair loss, crusts, nodules, discharge between toes
- Pain or limping; reluctance to walk
- Cracked pads, hyperpigmented skin.
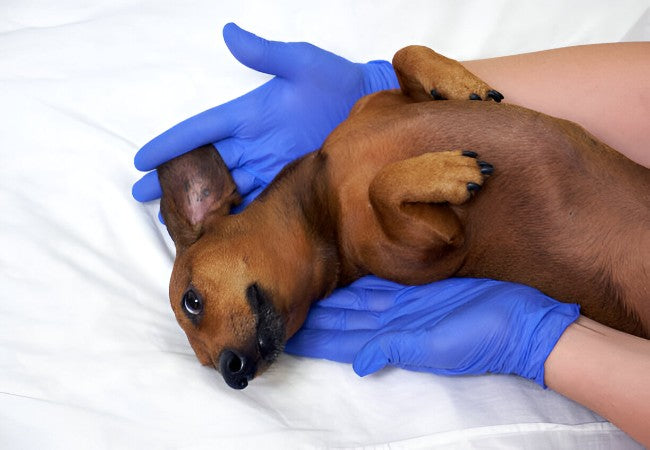
5. Diagnosing Pododermatitis
A thorough vet assessment includes:
- History & physical exam—evaluate paw hygiene, environment, dietary changes
- Skin cytology, hair plucks, scrapings—to detect bacteria, yeast, mites
- Cultures—bacterial/fungal to guide treatment
- Biopsy—especially for autoimmune lesions, tumors, chronic disease
- Bloodwork/endocrine testing—TSH, cortisol to assess hormonal roles
- Imagery—X-rays for bone tumors or foreign bodies.
6. Treatment Strategies
6.1. Addressing Infections
- Topical therapy—chlorhexidine, benzoyl peroxide, antifungal agents for localized lesions
- Systemic antibiotics (cephalexin, cefpodoxime, Convenia®) for deep or bacterial cases
- Antifungals or parasiticides for yeast or demodex infections.
6.2. Controlling Allergies
- Hypoallergenic diets or food elimination trials
- Allergy meds—antihistamines, steroids, cyclosporine, Apoquel®, Cytopoint®
- Booties or gloves to minimize contact allergens.
6.3. Immune-Mediated, Hormonal & Tumors
- Immune suppressants like steroids and azathioprine for pemphigus
- Treat hormonal conditions—thyroid or adrenal therapy
- Surgery, chemotherapy, or radiation for tumor-related pododermatitis.
7. Managing Chronic or Recurrent Cases
Chronic pododermatitis requires lifelong management, regular follow-up, and any combination of topical, systemic, and adjunctive care—often months before full resolution.
8. Prevention & Home Care
- 🔍 Inspect paws regularly for changes
- 🧼 Clean and dry between toes after walks; use antiseptic wipes
- 👟 Use booties in abrasive or allergen-prone environments
- ✂️ Trim hair between pads, nails, overgrown fur
- 🍽️ Maintain a healthy weight and balanced diet (omega-3s support skin healing)
9. Tools for Comfort & Enrichment
-
- Ask A Vet App: Remote follow-up, medication reviews, and treatment adjustments
10. Vet Case Example
Case: Bella, a 5‑year‑old Labrador
Bella presented with red, itchy paws between toes, chewing nonstop. Cytology showed yeast; cultures guided antifungal and antibiotic therapy. Care included daily chlorhexidine soaks, hoof trimming, APOQ chews, Cytopoint injections, and booties for grass allergy season. After 8 weeks, lesions resolved. Ongoing prevention includes an omega‑3 diet, seasonal allergy management, and Ask A Vet for flare‑ups.
11. Prognosis & Follow‑Up
- Infections—good to excellent with proper medication
- Allergy/hormone/tumor-related—managed, not always cured
- Regular reassessment—every 4–8 weeks during active therapy, then seasonally
📌 Final Thoughts from a Vet
Pododermatitis isn't just sore paws—it’s a symptom of deeper issues requiring systematic evaluation. With diagnosis-driven therapy, ongoing paw care, enrichment tools, and Ask A Vet telehealth support, many dogs live pain-free and active. Paw inflammation deserves thorough attention and a tailored care plan—your pup’s comfort is worth every step. 🐾❤️